The Best Way To Treat Hyperpigmentation According To Dermatologists
Megan Kelly
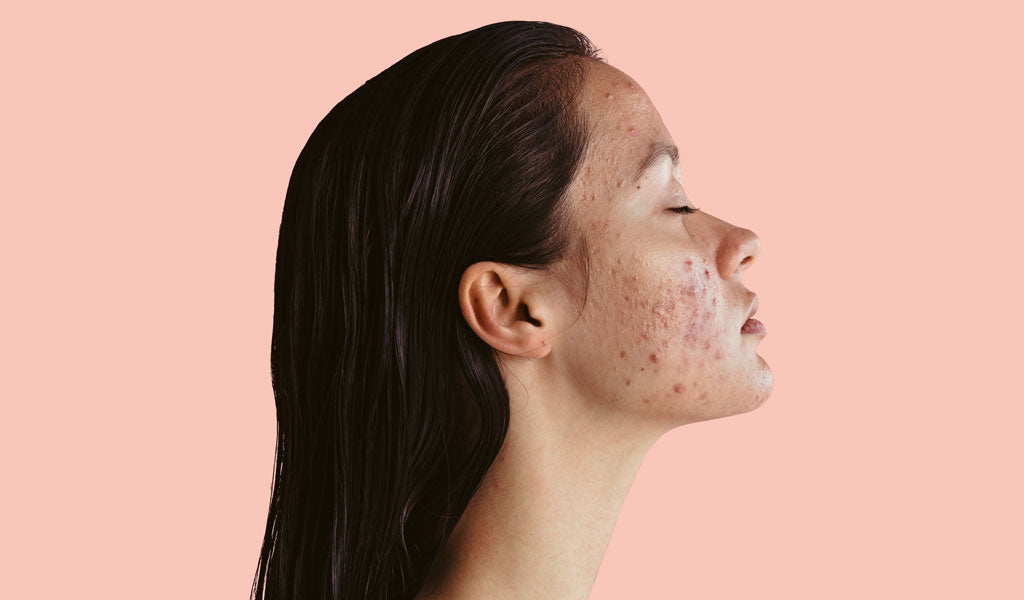
Hyperpigmentation is one of the skin concerns we hear about most from our community. It’s very common and can be very tricky to treat. (A not-very-fun combination, tbh.)
So, we’ve called in some two expert dermatologists to talk us through it all. Grab a snack and get comfy, we’re diving into the big wide world of hyperpigmentation.
What is hyperpigmentation and what are the main causes?
“Hyperpigmentation is the result of excess melanin production that forms deposits on our skin. Hyperpigmentation appears as darkened patches or spots on the skin that make skin look uneven,” says dermatologist Dr. Davin Lim.
Now here’s where it gets a little more confusing. Because there’s just not one type or cause of hyperpigmentation. Not even close.
“A number of factors can trigger an increase in melanin production, but the main ones are sun exposure, hormonal influences, age and skin injuries or inflammation,” explains Dr. Lim. Genetics is also widely recognised to be a key contributor to hyperpigmentation (which means you can blame it on Dad).
What are the different kinds of hyperpigmentation?
Now that we know what hyperpigmentation is generally speaking, let’s dig into what kinds of hyperpigmentation exist to help you identify what you’re dealing with.
“There are a myriad of [types and] causes of facial hyperpigmentation, with melasma and post-inflammatory hyperpigmentation being the commonest,” says dermatologist Dr. Katherine Armour.
Here is a breakdown of the most common.
Melasma: Probably the one you’ve heard the most about and one of the toughest ones to treat. Melasma is a skin disease that can be caused by many, many things.
“Melasma is a complex disease, with multifactorial mechanisms leading to its development. These include genetic predisposition, solar damage, skin barrier abnormalities, hormonal influences, and inflammation,” explains Dr. Armour, noting that a strong family history is very common when it comes to melasma and it’s more common amongst women who take the oral contraceptive pill, are pregnant, or with the use of hormone replacement therapy.
If you have melasma, be sure to take it easy on your skin, staying away from anything that could irritate your skin further. “It is crucial to avoid inflaming the skin with any of our treatments for melasma, as this can potentially worsen the condition,” advises Dr. Armour.
Post-Inflammatory Hyperpigmentation (PIH): If you’ve struggled with any form of skin inflammation, there’s a good chance you're familiar with Post-Inflammatory Hyperpigmentation, or PIH, as it’s commonly referred to.
As the name suggests, PIH is a (deeply annoying) farewell gift that’s left behind when you finally manage to calm down whatever was causing the inflammation in the first place. “This includes a variety of rashes (psoriasis, eczema, discoid lupus, or lichen planus) or traumas to the skin (overvigrous laser treatments or other injuries),” says Dr. Armour, explaining that you can expect to see PIH in the spots your face was inflamed.
You know when you get a pimple that hands around for a few days and then leaves behind a dark spot for weeks? That’s PIH. Which makes it also quite common amongst anyone with congested or acne-prone skin.
Lentigines: Also known as liver spots or age spots, lentigines appear due to prolonged sun exposure.
“These are essentially sun-induced freckles; they are often referred to as ‘pigmentation’ by the general public,” explains Dr. Armour. Lentigines will be clearly defined and can vary in size and are most common on our face, hands, and arms.
How to prevent hyperpigmentation
While different forms of hyperpigmentation are caused by things out of our control (genetics, age, etc.), that’s not to say there’s nothing you can do to help protect your skin.
“The most important way to prevent the development of facial hyperpigmentation caused by melasma and PIH is to protect every single day against ultraviolet and visible light,” says Dr. Amour, recommending that you find a broad-spectrum UVA and UVB blocking sunscreen that you love and wear it daily.
How to treat hyperpigmentation
“Ideally a diagnosis of the cause of pigmentation should be given prior to any treatments,” says Dr. Lim, adding that the best way to tackle pigmentation will consist of a combo of “topicals, peels, and lasers”.
Recommended topical ingredients include Niacinamide (Vit B3), Acids (Ascorbic, Lactic, Azelaic, Kojic, Tranexamic), Licorice, Retinol and Retinoids (Vit A such as Tretinoin) and Hydroquinone (formulated above 2%), which is often considered to be the best but also the most controversial topical for treating hyperpigmentation, so of course, seek your own advice from a GP or dermatologist before proceeding. And if you’re after an alternative? Botanical plant extracts (bearberry, blueberry and other ‘berries’) are accepted to be mainstream alternatives to hydroquinone, advises Dr. Lim.
In-clinic treatments, such as chemical peels can also be an enormous help when used in combination with topical treatments for melasma and PIH. “They are used to improve hyperpigmentation via a controlled exfoliation,” says Dr. Armour. “ Each ingredient in the peel is very carefully chosen to optimise the effectiveness, but also to reduce the risk of PIH.” Noting that sun protection is essential for anyone who has a course of chemical peels to prevent further damage.
Laser and light therapy are also a very popular in-clinic option to treat melasma, but Dr. Amour warns that while “numerous lasers and lights have been used in clinical trials to treat melasma”, they are not without risk, as if they are done incorrectly, it can actually worsen melasma or cause PIH. “Seeing a dermatologist who is experienced in the treatment of facial pigmentary disorders is really important if you are considering laser treatment for your melasma to ensure that your condition isn’t exacerbated,” says Dr. Armour. “They can advise which devices are most appropriate for your skin type.”



